CDC Issues Warning on Candida Auris, a Highly Drug Resistant and Dangerous Yeast Infection - DARKDaily.com - Laboratory News
CDC advises clinical laboratories and microbiologists encountering C. auris to follow their own protocols before adopting federal agency guidelines
In July, the Centers for Disease Control and Prevention (CDC) warned healthcare facilities and clinical laboratories to be on the alert for Candida auris (C. auris) infections in their patients. An outbreak of the drug resistant and potentially deadly fungus had appeared in two Dallas hospitals and a Washington D.C. nursing home.
Since those outbreaks, researchers have studied with urgency the "superbug's" emergence in various types of healthcare facilities around the nation, not just hospitals. Their goal was to discover how it was successfully identified and contained.
One such recently released study involved researchers from the Orange County Health Department (OCHD) working with the California Department of Public Health and the CDC to track C. auris in long-term acute care hospitals (LTACHs) and ventilator-capable skilled-nursing facilities (vSNFs), Medscape reported.
The researchers published their findings in Annals of Internal Medicine, titled, "Rapid Assessment and Containment of Candida auris Transmission in Post-acute Care Settings—Orange County, California, 2019."
"Seeing what was happening in New York, New Jersey, and Illinois [was] pretty alarming for a lot of the health officials in California [who] know that LTACHs are high-risk facilities because they take care of [very] sick people. Some of those people are there for a very long time," the study's lead author Ellora Karmarkar, MD, MSc, told Medscape. Karmarkar is an infectious disease fellow with the University of Washington and formerly an epidemic intelligence service officer with the CDC.
"One of the challenges was that people were so focused on COVID that they forgot about the MDROs (multi-drug resistant organisms] … Some of the things that we recommend to help control Candida auris are also excellent practices for every other organism including COVID care," she added.
According to Medscape, "The OCHD researchers screened LTACH and vSNF patients with composite cultures from the axilla-groin or nasal swabs. Screening was undertaken because 5%–10% of colonized patients later develop invasive infections, and 30%–60% die.
Medscape also reported that the first bloodstream infection was detected in May 2019, and that, according to the Annals of Internal Medicine study, as of January 1, 2020, of 182 patients:
- 22 (12%) died within 30 days of C. auris identification,
- 47 (26%) died within 90 days,
- One of 47 deaths was attributed to C. auris,
- Whole-genome sequencing showed that the isolates were all closely related in clade III.
"This is really the first time we've seen clustering of resistance in which patients seemed to be getting the infections from each other," Meghan Lyman, MD, Medical Officer in the Mycotic Diseases Branch of the CDC, told Fox News.
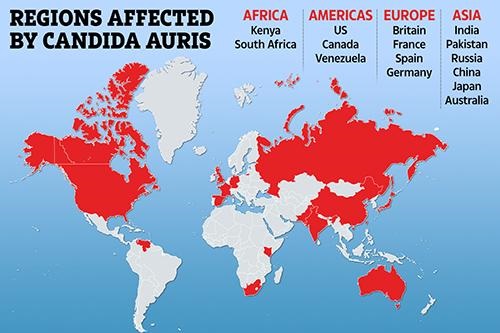
The graphic above illustrates how Candida auris is "spanning the globe," The New York Times reported. Clinical laboratories that encounter this potentially deadly fungus are advised to contact the CDC immediately for guidance and to take proactive steps to prepare for the "superbug's" arrival. (Graphic copyright: The Scottish Sun.)
Be More Proactive than Reactive in Identifying C. Auris, CDC Says
C. auris is a type of yeast infection that can enter the bloodstream, spread throughout the body, and cause serious complications. People who appear to have the highest risk of contracting the infection are those:
- Who have had a lengthy stay in a healthcare facility,
- Individuals connected to a central venous catheter or other medical tubes, such as breathing or feeding tubes, or
- Have previously received antibiotics or antifungal medications.
The CDC is concerned about C. auris for three primary reasons:
- It tends to be resistant to the antifungal drugs that are commonly used to treat Candida infections.
- It can be difficult to identify via standard laboratory testing and is easily misidentified in labs without specific technology.
- It can quickly lead to outbreaks in healthcare settings.
"With all this spread that we've been seeing across the country we're really encouraging health departments and facilities to be more proactive instead of reactive to identifying Candida auris in general," Lyman told STAT. "Because we've found that controlling the situation and containing spread is really easiest when it's identified early before there's widespread transmission."

There continues to be concerns over this highly drug-resistant infection among hospital physicians and medical laboratories. "Acute care hospitals really ought to be moving toward doing species identification of Candida from nonsterile sites if they really want to have a better chance of detecting this early," Dan Diekema, MD (above), an epidemiologist and clinical microbiologist at the University of Iowa, told Medscape. (Photo copyright: University of Iowa.)
Candia Auris versus Other Candida Infections
C. auris can cause dangerous infections in the bloodstream and spread to the central nervous system, kidneys, liver, spleen, bones, muscles, and joints. It spreads mostly in long-term healthcare facilities among patients with other medical conditions.
The symptoms of having a Candida auris infection include:
- Fever
- Chills
- Pain
- Redness and swelling
- Fluid drainage (if an incision or wound is present)
- General feeling of tiredness and malaise
C. auris infections are typically diagnosed via cultures of blood or other bodily fluids, but they are difficult to distinguish from more common types of Candida infections, and special clinical laboratory tests are needed to definitively diagnose C. auris.
Whole-genome Sequencing of C. Auris and Drug Resistance
The CDC conducted whole-genome sequencing of C. auris specimens gathered in Asia, Africa, and South America and discovered four different strains of the potentially life-threatening Candida species. All four detected strains have been found in the United States.
There are only three classes of antifungal drugs used to treat Candida auris infections:
However, 85% of the infections in the US have proven to be resistant to azoles and 38% are resistant to polyenes. Patients respond well to echinocandins, but more effective therapies are needed especially as some isolates may become resistant while a patient is on drug therapy, STAT reported.
"Even while it might be susceptible upfront, after a week or two of therapy, we may find that the patient has an infection now caused by an isolate of the same Candida auris that has become resistant to the echinocandins and we are really left with nothing else," Jeffrey Rybak, PhD, PharmD, Instructor, Department of Pharmaceutical Sciences, St. Jude Children's Research Hospital, told Infection Control Today.
Although relatively rare, C. auris infections are on the rise. The good news is that there may be further pharmaceutical help available soon. New antifungal agents, such as Ibrexafungerp (Brexafemme) show promise in fighting C. auris infections, but more research is needed to prove their efficacy.
What Should Clinical Laboratories Do?
The CDC stresses that clinical laboratories and microbiologists working with known or suspected cases of Candida auris should first adhere to their own safety procedures. The CDC issued guidelines, but they are not meant to supersede the policies of individual labs.
The CDC also recommends that healthcare facilities and clinical laboratories that suspect they have a patient with a Candida auris infection immediately contact the CDC and state or local public health authorities for guidance.
—JP Schlingman
Related Information
U.S. Sees First Cases of Dangerous Fungus Resistant to all Drugs in Untreated People
'Superbug' Fungus Spread in Two Cities, Health Officials Say
CDC: Candida auris
CDC: Drug-resistant Candida auris
CDC Reports Two Outbreaks of Pan-resistant Candida auris
Notes from the Field: Transmission of Pan-Resistant and Echinocandin-Resistant Candida auris in Health Care Facilities―Texas and the District of Columbia, January–April 2021
Drugs in Development Might Help Fight Deadly Candida Auris
During Pandemic, Clinical Laboratories Should Be Alert for Drug Resistant Infections That Pose High Risk to COVID-19 Patients
Potentially Fatal Fungus Invades Hospitals and Public Is Not Informed
Comments
Post a Comment